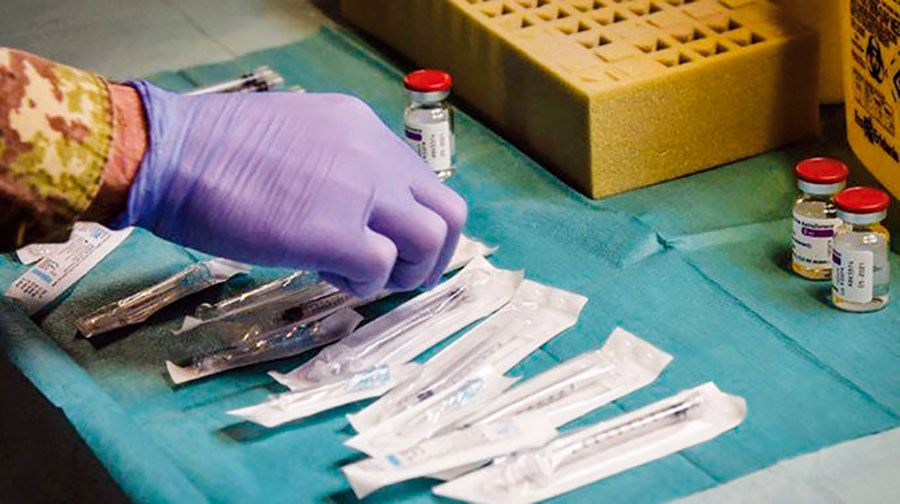
Antibiotic use in Uganda is high: action is needed
Even before the COVID crisis, excessive use and misuse of lifesaving antibiotics had contributed to the emergence of resistant strains of disease-causing organisms. This has rendered many of the most powerful treatments in modern medicine ineffective.
It’s estimated that drug-resistant infections caused more than 1.2 million deaths in 2019. That is more than malaria and AIDS combined. And resistance contributed to about 5 million additional deaths.
There’s some evidence that the COVID-19 pandemic made matters worse.
COVID-19 is caused by a virus. And viruses are not treated with antibiotics. But early treatment guidelines for COVID-19 assumed that patients admitted to hospitals would develop bacterial superinfections that required antibiotics. The sheer volume of people who were sick with respiratory infections also seemed to encourage additional use of antimicrobial drugs.
Antimicrobials are drugs that treat bacterial, viral or other microbial infections. Antimicrobial resistance, the drop in effectiveness of this broader class of drugs, was already a rising threat to global public health before December 2019.
In general, sub-Saharan Africa suffers from the highest rate of drug resistance-related deaths. But the prevalence varies by country. In our recent research we set out to document the magnitude of antimicrobial use, a known driver of antimicrobial resistance, in selected healthcare facilities in Uganda.
We found a high use of antibiotics across all surveyed health facilities. And compliance to Uganda’s clinical guidelines among healthcare workers was low. Also, men were more likely to be on antibiotics than women. In addition, antibiotic use was two times higher in public health facilities than in the private sector. But this could be attributed to the higher proportion of public healthcare facilities in our study sample.
Our results highlight areas for intervention to address antimicrobial resistance. These findings also provide a baseline against which we can compare the impact of such interventions.
Trends in antibiotic use
We surveyed antibiotic use in 13 hospitals in Uganda. Our analysis included nearly 1,100 patients and was done between December 2020 and April 2021.
Nearly three-quarters of all patients in our study were taking at least one antibiotic. This is high and could indicate overuse, some of which may be unnecessary. In addition less than 30% of the antibiotic prescriptions complied with Uganda’s clinical guidelines for choice of drugs.
Ceftriaxone is a drug used to manage a wide range of infections. It was among the most prescribed antimicrobials. But it’s not recommended for first-line use. A possible explanation for this is convenience and ease of its use as compared to the current first-line medicines. Read More…