There's no cure for sickle cell disease, but spotting it early can improve treatment
What is sickle cell disease?
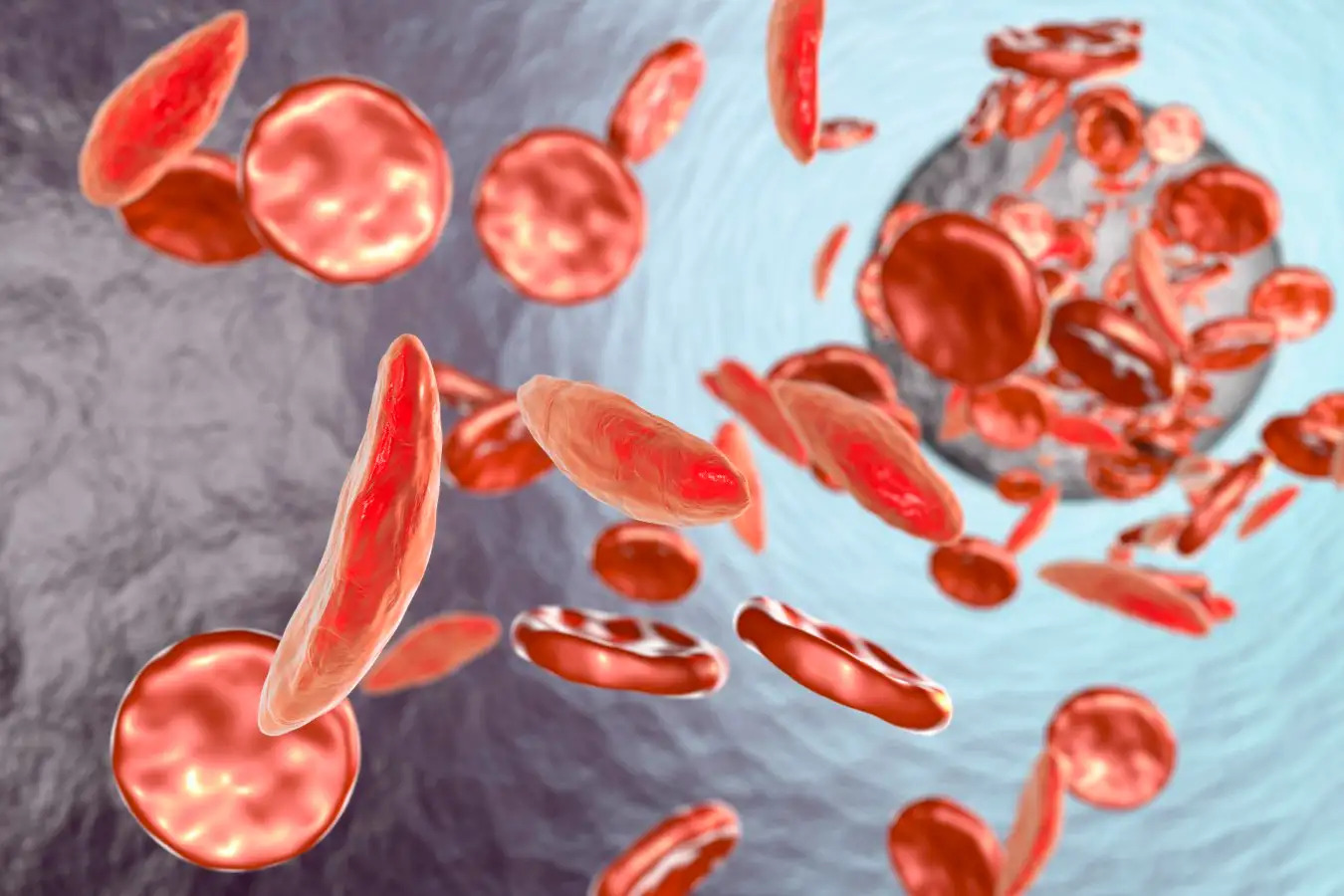
Sickle cell disease is a genetic disorder that causes misshapen red blood cells to clog blood vessels. The condition can cause extreme pain. People with sickle cell disease are at risk of life-threatening infections. These include pneumonia and meningitis. They are also at risk of other complications such as stroke or loss of vision. If left untreated, sickle cell disease can prove fatal. As a genetic condition, the disease is not preventable. But it can be managed with the proper treatment. Treatment is more effective if the disease is detected early in life.
The disease is a consequence of a gene mutation that granted a degree of protection against the threat of malaria. Research suggests the mutation originated in a single child in Africa roughly 7,300 years ago. It’s thought that the gene could limit the ability of the malaria parasite to infect host cells. The descendants of this child, with a greater resistance to malaria than those without the sickle cell trait, spread across the globe. Today, people with the gene are found in greater numbers in areas prone to malaria, such as sub-Saharan Africa.
When two individuals with the mutation pass copies of the gene to their child, the child will have sickle cell disease rather than sickle cell trait, and will not have the same resistance to malaria.
Those with the disorder are actually at higher risk of severe illness if admitted to hospital for malaria today.
How big is sickle cell disease in Africa?
An estimated 20 million people live with sickle cell disease globally. More than 66% of them are in sub-Saharan Africa. Around 300,000 children are born with sickle cell disease globally every year. Three out of four of these children are born in a geographic belt from Senegal to Madagascar – translating to 1%-3% of children born in this belt. Countries in Africa with the highest prevalence are Cameroon, Nigeria, the Democratic Republic of Congo and Ghana.
What measures are in place to manage it?
Just a few short decades ago, it was common for children with undiagnosed sickle cell disease to die from severe infections. But these cases are reducing with improvements in research and science. Newborn screening is preferable to testing following symptoms.
Early diagnosis, preventive care and active clinical management can prevent complications and death, and improve quality of life. If we know a child has sickle cell disease right from birth, we can put in place measures such as prophylaxis (screening for stroke or silent brain infarcts and starting disease modifying drugs such as hydroxyurea,annual assessment of organ function (liver and kidneys) and use antibiotics when required to ensure that severe infectious diseases do not occur. Read More…